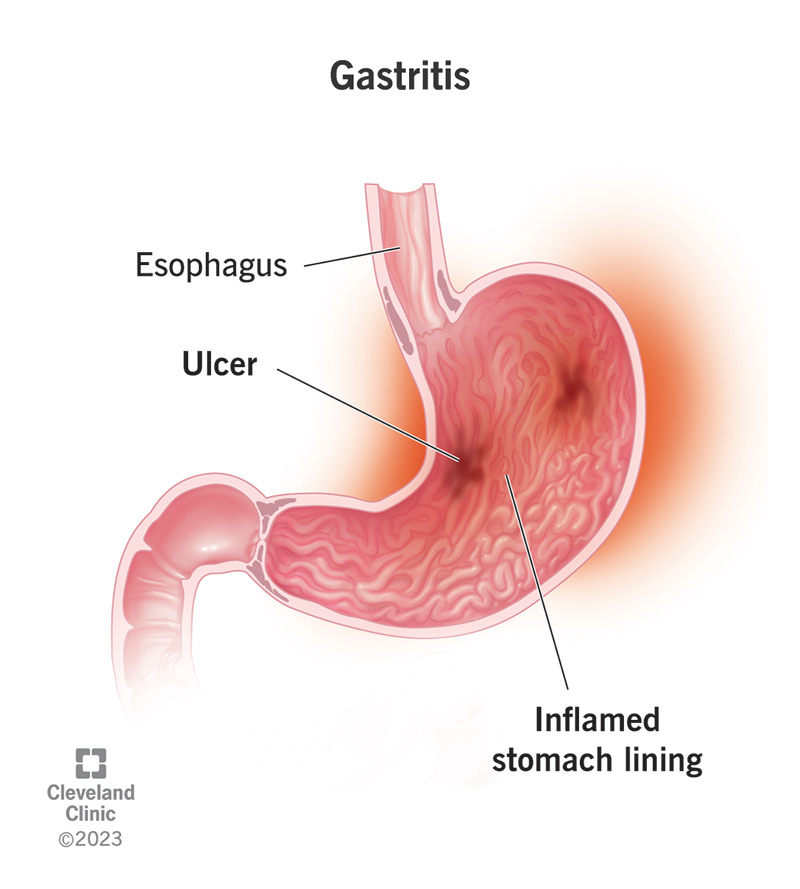
Burning Stomach Pain After Eating: Causes, Gastritis, and Relief
Burning stomach pain after eating is one of the most recognizable digestive symptoms — yet it can also be confusing. Many people assume it means acid reflux or ulcers, but in many cases the burning sensation actually comes from irritation of the stomach lining.
In my own recovery experience, this symptom didn’t appear immediately. It developed after a period of milder upper abdominal discomfort and sensitivity to meals. That progression is very typical of gastritis-related irritation.
Why Burning Pain Happens After Eating
After a meal, the stomach naturally produces acid and digestive enzymes. When the stomach lining is healthy, this process causes no discomfort. But if the lining is irritated or inflamed, acid contact can trigger a burning sensation.

This is why burning stomach pain often begins shortly after eating rather than on an empty stomach. If you're unsure about the exact location of gastritis discomfort, see where gastritis pain is felt.
Common Causes of Burning Stomach Pain After Meals
👉 Ultimate Guide to Gastritis1. Gastritis
The most common cause is inflammation or irritation of the stomach lining. When food and acid contact the sensitive surface, a burning sensation develops. Learn more about common causes of gastritis.
2. Acid sensitivity
Even normal acid levels can feel excessive if the stomach lining is already irritated. This explains why mild meals can still trigger burning.
3. Trigger foods
Certain foods increase irritation or acid activity, including:
- Fried or fatty meals
- Spicy foods
- Coffee
- Alcohol
- Acidic foods
During my gastritis phase, coffee and oily meals consistently triggered burning within 20–30 minutes.
4. Stress-related stomach sensitivity
Stress changes stomach acid regulation and increases nerve sensitivity. If stress plays a role, read can stress cause gastritis.
How Gastritis Burning Feels Different From Reflux
People often confuse gastritis burning with acid reflux, but they feel different:
- Gastritis: burning in upper abdomen after eating
- Reflux: burning rising toward chest or throat
This distinction helped me understand that my symptoms were stomach-based rather than esophageal.
When Burning Pain Starts After Eating
Timing gives clues about cause:
- Immediately after eating: stomach lining irritation
- 30–60 minutes: acid contact with inflamed lining
- 2–3 hours: delayed emptying or acid exposure
My symptoms typically appeared about 20–40 minutes after meals, especially larger ones.
Is Burning Stomach Pain Serious?
Most cases are related to gastritis or temporary irritation and improve with dietary and lifestyle changes. However, persistent burning should be medically evaluated.
Seek medical care if burning:
- Occurs daily
- Worsens over weeks
- Occurs with vomiting
- Includes weight loss or bleeding
Relief Strategies That Helped Me
These steps consistently reduced burning stomach pain during recovery:
- Smaller meals
- Low-fat foods
- Avoiding coffee temporarily
- Warm (not hot) foods
- Slow eating
Interestingly, meal size mattered more than food type early in healing. Even safe foods triggered burning when portions were large.
Key Takeaway
Burning stomach pain after eating most often reflects stomach lining irritation rather than severe disease. It commonly appears during gastritis and improves as the lining heals.
Recognizing triggers and adjusting meal patterns can significantly reduce symptoms and support recovery.
Medical Disclaimer: This article is for educational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider regarding digestive symptoms.
Sources: Clinical gastroenterology references, gastritis and dyspepsia research literature, and medical education resources on upper gastrointestinal symptoms.
Privacy Policy | Terms of Service | Contact | About the Author
📚 Complete Gastritis Resource Center
Explore our full evidence-based guide covering symptoms, causes, progression, and recovery strategies for gastritis.
🔎 Symptoms & Pain Location
- Where Is Gastritis Pain Felt?
- Upper Abdominal Discomfort Explained
- Chest Tightness & Gastritis
- Nighttime Gastritis Symptoms
- Frequent Burping & Gastritis
- Loss of Appetite & Gastritis
- Nausea and Gastritis
- Early Warning Signs
⚡ Causes & Triggers
- Common Causes of Gastritis
- Medication-Induced Gastritis
- Alcohol-Related Gastritis
- Can Stress Cause Gastritis?
- Lifestyle Triggers
- How Age Affects Risk
- Gastritis in Young Adults
📊 Types & Progression
- Acute vs Chronic Gastritis
- When Gastritis Becomes Chronic
- Mild vs Severe Gastritis
- How Gastritis Develops
- Gastritis Without Pain
🛡 Prevention & Recovery
- Can Gastritis Be Prevented?
- Understanding the Stomach Lining
- What Doctors Mean by Stomach Inflammation
- Morning Stomach Pain Causes
- Bloating After Meals
Main Hub: Return to GutReliefHub Home